What is hallux abducto valgus (bunions) and what causes it?
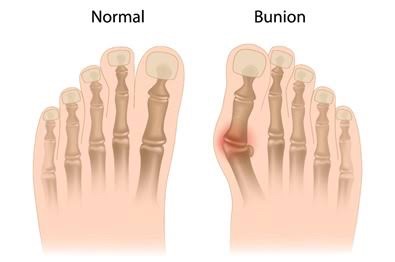
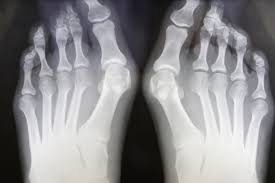
Hallux abducto valgus, or bunions as it’s more commonly called, is the most common deformity of the forefoot (Wulker & Mittaf 2012). It is characterised by a deviation of the great toe resulting in deformity and malpositioning of the metatarsophalangeal joint (Fraisslet et al. 2016).
Often the reason for the development of HAV in individual cases can be hard to define. However, familial inheritance, inappropriate footwear (narrow, pointed, and high heel shoes), flat feet, and gender play significant roles in the development of HAV (Perera, Mason & Stephens 2011; Wulker & Mittaf 2012). Depending on the stage of HAV development it can cause pain and impact activities of daily living, particularly in its later stages. For this reason it is recommended treatment is sought out as soon as possible
Who does hallux abducto valgus affect?
Hallux abducto valgus is the most common condition of the forefoot and it is reported that up to 35% of the world’s population is affected by hallux valgus (Nix, Smith, & Vicenzino 2010). The prevalence of hallux abducto valgus increases with age, and is most common amongst those aged 65 years or older, affecting 35% of this demographic. It is slightly less prevalent in those aged between 18-65 years, but still affects an estimated 23% of this population (Nix, Smith, & Vicenzino 2010). Gender also plays a role in the incidence of hallux abducto valgus, with a higher incidence of women developing the condition than men. This increased incidence has been reported as high as 15:1 (women:men) in some studies and is believed to associated with differences in womens footwear choices and higher rates of ligamentous laxity (Hecht & Lin 2014; Perera, Mason & Stephens 2011).
What are the symptoms of hallux abducto valgus?
Three stages of hallux abducto valgus development (mild, moderate, and severe) are often described amongst clinicians (ICB Medical). Symptoms of hallux abducto valgus will depend on the stage of the condition.
Primary stage (mild) – Typically at this stage symptoms are minimal. Patients may notice the early formation of a ‘bump’ on the inside of their great toe. This is that beging of the hallux abducto valgus formation (Talbot 2018).
Secondary stage (moderate) – In this stage the great toe will begin to deviate towards the outside of the body, and the metatarsal bone may begin to deviate towards the inside of the body. It is at this stage that pain and irritation from footwear begins (Talbot 2018).
Tertiary stage (severe) – This is the most severe stage of hallux abducto valgus. At the tertiary stage the great toe will have deviated significantly towards the outer side of the body, often over or underlapping the second and third toes. This stage will coincide with a significantly prominent, inflamed metatarsal head. Pain will be at its most significant and difficulties in walking and fitting shoes are expected (Ferrari 2014; Talbot 2018).
How do we treat hallux abducto valgus?
Hallux abducto valgus can be treated either non-operatively or operatively depending on the degree of deformity and symptoms.
Unfortunately, non-operative treatments will not correct the degree of deformity, but can help in alleviating symptoms (Fraisslet et al. 2016). Conservative and non-operative treatment methods should be trialled initially, and utilised where surgery is a contraindication such as in those with peripheral arterial disease etc. Non-surgical treatments may include, footwear modifications including a wider fitting toe-box, paddings or shields to protect the painful bony prominence, night splinting, or custom orthotic devices to improve foot mechanics and reduce bunion progression (Fraisslet et al. 2016).
In severe cases, or cases where conservative treatment methods have not alleviated symptoms operative treatment may be recommended. There have been more than 100 different surgical techniques described for the correction of hallux abducto valgus. A suitable surgical technique is chosen depending on factors such as the degree of deformity, degenerative changes, and the size and shape of the metatarsal bone (Fraisslet et al. 2016).
References
Ferrari, J 2014, ‘Hallux valgus (bunions), BMJ Clinical Evidence, vol. 1112, no. 4, pp. 1-46.
Fraissler, L, Konrads, C, Hoberg, M, Rudert, M & Walcher, M 2016, ‘Treatment of hallux valgus deformity’, EFORT Open Reviews, vol. 8, no. 1, pp. 295-302.
Hecht, PJ & Lin, TJ 2014, ‘Hallux Valgus’, Medical Clinics of North America, vol. 98, no. 2, pp. 227-232.
ICB Medical, Bunions (Hallux Abducto Valgus), ICB Superior Biomechanics, viewed 15 May 2019, <https://www.icbmedical.com/bunions.php>.
Nix, S, Smith, M & Vicenzino, B 2010, ‘Prevalence of hallux valgus in the general population: a systematic review and meta-analysis’, Journal of Foot and Ankle Research, vol. 21, no. 3, pp. 1-9.
Perera, AM, Mason, L & Stephens, MM 2011, ‘The Pathogenesis of Hallux Valgus’, Journal of Bone and Joint Surgery, vol. 93, no. 17, pp. 1650-1661.
Talbot, M 2018, Bunion – Do I have one on my big toe?, Foot & Leg Centre, viewed 15 May 2019, <https://www.footandleg.com.au/what-is-a-bunion/>.
Wulker, N & Mittaf, F 2012, ‘The Treatment of Hallux Valgus’, Deutsches Ärzteblatt International, vol. 109, no. 49, pp. 857-868.
