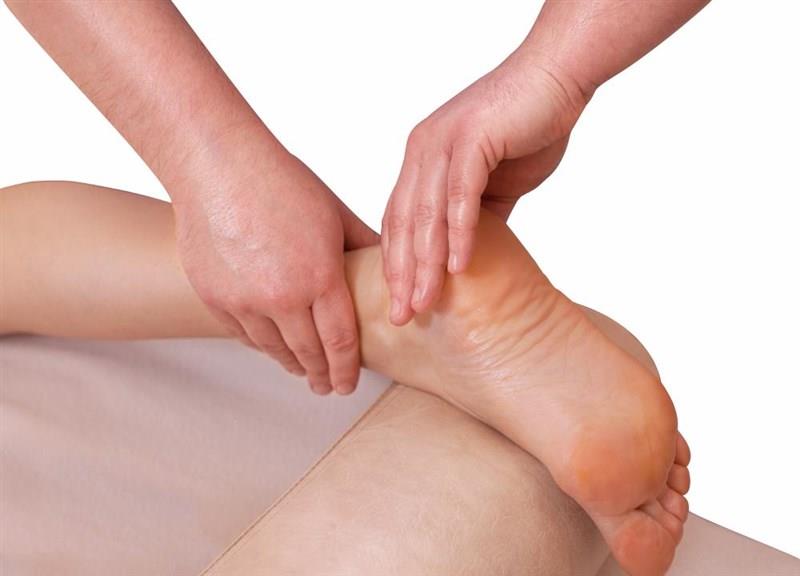
What is plantar fasciitis, and how is it caused?
Plantar fasciitis, or heel pain as it is more commonly called, is the inflammation or degeneration of a structure within the foot called the plantar fascia (Schwartz, 2014). Physiotherapists and podiatrists typically treat this condition with the best results from a team approach.
The plantar fascia is a thick fibrous band that extends from your heel to the base of your toes and supports the arch of your foot. It is thought that repetitive strain and spikes in load from long periods of standing or activity and a person’s foot type cause this painful inflammatory and tendinopathic condition (Schwartz, 2014).
Who does plantar fasciitis affect?
Plantar fasciitis is one of the most common causes of foot pain and is estimated to affect 1 in 10 people during their lifetime (Riddle, Pulisic, Pidcoe, & Johnson, 2003). Plantar fasciitis can affect people in sedentary and athletic populations and anyone in between (Schwartz, 2014). However, research indicates that the peak incidence of the condition is among those aged between 45 and 64 years and that it is more common among women. Those with excessively flat or high-arched feet are at an increased risk of developing plantar fasciitis (Riddle & Schappert, 2004).
What are the symptoms of plantar fasciitis?
Patients usually present with a gradual onset of pain at the medial or inner side of the heel (Lim, How, & Tam 2016). This pain is often described as ‘first step pain’ and presents as severe pain occurring with the first few steps after res, then improving with movement. However, the pain may be re-aggravated by long periods of weight-bearing (Schwartz, 2014). Clinically, plantar fasciitis is diagnosed by palpation of the plantar medial heel, resulting in tenderness and dorsiflexion of the first toe (Schwartz, 2014).
How do physiotherapists and podiatrists treat plantar fasciitis?
For most patients, plantar fasciitis can be treated conservatively and without surgical intervention (Lim, How, & Tam 2016). Conservative management of plantar fasciitis often requires several treatment modalities for the best chance of recovery. Some standard and evidence-based treatment methods include:
Avoidance of any repetitive and high-impact activities, only slowly returning to such once-asymptomatic activities for 4-6 weeks or gradually reloading the tissue (Lim, How, & Tam 2016),
Superficial plantar fascia and calf stretch, in combination with ic and massage (Lim, How, & Tam 2016).
Graduated Exercise Loading Programme
- Low dye provides the foot’s medial arch with some initial support (Schwartz, 2014).
- More appropriate and supportive footwear choices,
- Orthotic therapy is a longer-term treatment method (Cutts, Obi, Pasapula, & Chan 2012).
- Unfortunately, not all cases of plantar fasciitis respond to conservative management. Surgical intervention may be required in approximately 5% of patients (Lim, How, & Tam 2016).
References
Cutts S, Obi N, Pasapula C, and Chan W (2012), ‘Plantar Fasciitis’, Annals of the Royal College of Surgeons of England, vol. 94, no. 8, pp. 539–542.
Lim AT, How CH, and Tam B (2016), ‘Management of plantar fasciitis in the outpatient setting’, Singapore Medical Journal, vol. 57, no. 4, pp. 168–171.
Riddle DL, Pulisic M, Pidcoe P, & Johnson RE 2003, ‘Risk factors for plantar fasciitis: a matched case-control study’, Journal of Bone and Joint Surgery, vol. 85, pp. 872–7.
Riddle DL & Schappert SM 2004, ‘Volume of ambulatory care visits and patterns of care for patients diagnosed with plantar fasciitis: a national study of medical doctors’, Foot Ankle Int., vol. 25, no. 5, pp. 303–310.
Schwartz EN, 2014, ‘Plantar Fasciitis: A Concise Review’, The Permanente Journal, vol. 18, no. 1, pp. 105–107.