“I’ve got lots of muscle knots and trigger points,” “My neck is all knotted up; I can feel the trigger points,” and “My shoulders have so many knots and trigger points in them.” We hear these terms daily as physiotherapists, podiatrists, or massage therapists. However, what is a muscle knot or trigger point? What causes muscle knots and trigger points? How do we eliminate those pesky muscle knots and trigger points?
In this blog, I’ll discuss these hot topics, as muscle knots can be debilitating to patients, cause pain, inhibit performance, and mimic other conditions through particular referral patterns.
What are muscle knots or muscle trigger points?
Let’s start with the basics: what is a muscle knot or a muscle trigger point? First, a muscle knot is a colloquial term for the more scientific myofascial trigger point. Myofascial trigger points, also known as muscle knots, are lumps in a tight band of skeletal muscle that can be very painful when they are not supposed to be (active trigger points). In contrast, some muscle trigger points are only painful when squeezed or compressed (latent trigger points). These trigger points can lead to muscle dysfunction, pain, weakness, and a loss of range of movement.
Types of Myofascial Trigger Points
- Primary or central TrPs cause severe pain locally at the pressure of irradiation, according to the referred pain map. Usually, they are based around the centre of a muscle belly.
- Secondary or satellite TrPs arise in response to existing central trigger points in surrounding muscles. They usually spontaneously withdraw when the central TrP is healed. It can be present in the form of a cluster.
These muscle knots, or trigger points, can often lead to myofascial pain syndrome. Myofascial pain syndrome can be acute or chronic and involves the muscles and their surrounding connective tissue, such as fascia; it can also lead to muscle sensitisation of the nerve tissue in the area and some visceral interactions (interactions between pain produced by skin and muscle and those of the organ system). Figure 1. Area cellular image of a series of trigger points
What causes muscle knots or muscle trigger points to form?
Muscle knots or muscle trigger points form for several reasons, usually caused by overuse or trauma. However, our bodies are complete and can form due to psychological stressors. Sustained postures or repetitive activities can cause enough stress in tissues that they can create trigger points or knots in muscles and can begin to elicit pain.
Summary of Why Trigger Points Can Form:
- Aging
- Injury sustained by a fall, stress, or birth trauma
- Lack of exercise is common in sedentary persons between 27 and 55 years old, of whom 45% are men
- Bad posture: upper and lower crossed pattern, swayback posture, telephone posture, cross-legged sitting,
- Muscle overuse and respective micro-trauma—weightlifting,
- Chronic stress conditions: anxiety, depression, and psychological stress trauma,
- Vitamin deficiencies: vitamin C, D, and B; folic acid; iron;
- Sleep disturbance,
- Joint problems and hypermobility
Why Do Muscle Knots and Muscle Trigger Points Become Painful?
This is an excellent question! The true nature of this answer is a bit ambiguous. Depending on the research you read, there are a few main competing theories. The first involves the small areas of the muscle becoming tight, like a microcrack in an area of strength. As this fast patch of muscle increases over time, it begins to receive a reduction in blood supply, which makes the tissue more irritable; in the research, it is referred to as experiencing a ‘metabolic crisis.’
Another idea is that the tissue area in question only experiences a sensory disturbance. This means that the nerves in that area (peripheral nervous tissue) receive input or stimuli (mechanical or chemical) that cause pain.
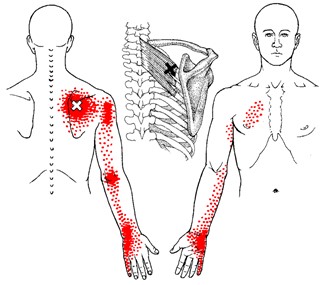
It is, however, essential to understand that active trigger points and muscle knots don’t just respond to pressure pain. They can painfully ache and induce muscle stiffness that spreads out and around a central muscle trigger point. These trigger points can spread and cause pain to all corresponding body areas when this occurs. Some experts in myofascial pain syndrome and referred pain are Travell, J.G., and Simons, DG, who in 1983 researched and produced a map of referred pain from myofascial trigger points called the trigger point manual. This is a text we, as clinicians, still refer to today in our practice and education!
Below is an example of referred pain from muscle knots or myofascial trigger points; however, we will explore referred pain in another blog piece!
What does it feel like to have myofascial trigger points or muscle knots?
Below is a list of general signs and symptoms of myofascial trigger points or muscle knots. You do not need to have all of them, but you will likely have a few combined.
- General sore spots, sensitive to pressure, primarily in muscles. (Pain where tendons are attached to joints is usually a different problem.)
- Pain is primarily dull, aching, and nagging.
- Your pain feels more like it’s in muscles than joints and seems deep.
- Affected limbs may feel a little weak, heavy, and stiff.
- Pain mainly occurs in a specific area with a reasonably straightforward epicentre. You can almost pinpoint it.
- There is no precise mechanism of injury, but flare-ups often occur due to extremes of position, exercise, or temperature.
- Pain is usually in episodes but can last for days, weeks, or months.
- The pain may move around a bit—even to the other side of your body! While uncommon, it’s a distinctive symptom of trigger points.
- You crave massage, but it usually provides only temporary relief.
- Hot showers, baths, and heat packs provide relief.
- You usually feel better with activity and exercise.
- The pain is not strongly or sharply linked to the movement (as an ankle sprain would be).
How do you treat and relieve myofascial trigger points and knots?
Now it’s time for the juicy stuff! How do we work to alleviate these pesky, irritable, and very annoying tight bits of muscle?
There are various ways to approach and treat this condition; some are very conservative, but there are more invasive forms of treatment for more severe, chronic trigger point conditions.
Physiotherapy and Myofascial Trigger Point Treatment
Usually, physiotherapy in Cheltenham is a very effective way of treating this condition. Physiotherapists have a variety of tools to approach this condition.
- Trigger point therapy, or ischemic compression, involves applying a firm, sustained pressure to the irritable trigger point to create a point of ischemia (lack of blood and oxygen supply). The goal is to free the sarcomeres (contracted muscle in the trigger point) to gradually relax the tension in the trigger zone. This can also be known as compression therapy or pressure therapy.
- Dry needling therapy is a procedure or treatment where your Physiotherapist inserts a fine acupuncture needle into the muscle aimed at myofascial trigger points. This stimulates a cascade of chemical release from the forces and can elicit a local twitch response with a contraction and relaxation of the muscle fibres in the contracted tissue, effectively releasing a significant amount of pain-causing chemicals within the trigger point.
- Massage
- Passive stretching techniques
- Taping techniques assist with decreasing muscle activation and supporting overworked tissue.
- Spray and stretch techniques with cold sprays to deactivate trigger points
- Heat and cold packs
- Education as to postures and positions that may contribute to the cause of trigger points
- Education as to self-release techniques you can use at home to assist in alleviating pain, muscle knots, and myofascial trigger points
Travell, J.G.; Simons, DG. Myofascial pain and dysfunction: the trigger point manual Williams & Wilkins; Baltimore: 1983. 10.
Travell JG, Rinzler SH. The myofascial genesis of pain. Postgraduate Medicine. 1952; 11:434–452.
Robert B. Myofascial Pain Syndromes and Their Evaluation Best Practise & Research Clinical Rheumatology. 2007; 21(3):427–445. [PubMed: 17602992]
Vázquez Delgado E, Cascos-Romero J, and Gay Escoda C. Myofascial pain associated with trigger points: a literature review, Part 2: differential diagnosis and treatment Medicina Oral, Patología Oral y Cirugia Bucal, 2010, vol. 15, num. 4, p. 639–643. 2010 July 1
Paul Ingraham, The Complete Guide to Trigger Points and Myofascial Pain, https://www.painscience.com/tutorials/trigger-points.php, November 2020.