What is POTS or Postural Orthostatic Tachycardia Syndrome?
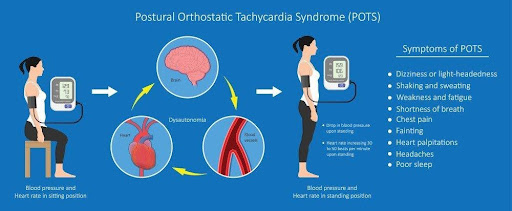
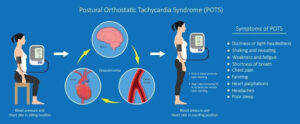 Postural Orthostatic Tachycardia Syndrome (POTS) is a complex medical condition of the autonomic nervous system characterized by a rapid increase in heart rate upon transitioning from a reclined or seated position to standing. The sudden increase in heart rate is a response made to try to correct the drop in blood pressure occurring with postural hypotension. Often this increase in heart rate is a useful adaption to try and get more blood circulating around the body. However, the problem is that the response is out of proportion to what is needed, causing a tachycardiac response (heart rate over 100 beats per minute) and a cascade of other symptoms.
Postural Orthostatic Tachycardia Syndrome (POTS) is a complex medical condition of the autonomic nervous system characterized by a rapid increase in heart rate upon transitioning from a reclined or seated position to standing. The sudden increase in heart rate is a response made to try to correct the drop in blood pressure occurring with postural hypotension. Often this increase in heart rate is a useful adaption to try and get more blood circulating around the body. However, the problem is that the response is out of proportion to what is needed, causing a tachycardiac response (heart rate over 100 beats per minute) and a cascade of other symptoms.
To be diagnosed with Postural Orthostatic Tachycardia Syndrome, the heart rate must have increased by >30 bpm from a resting heart rate within 10 minutes of standing.
In addition to the heart rate changes as a result of the postural change, people who have POTS will usually have smaller hearts and less blood volume compared to people without the condition. This affects cardiovascular health and fitness, as well as the ability to perform common daily tasks. POTS can therefore lead to a variety of debilitating symptoms impacting an individual’s life on a day to day basis. Severely affected individuals are unable to work, attend school or participate in recreational activities.
Symptoms of POTS
 While the hallmark symptom is the increase in heart rate, POTS is a collection of symptoms. These include:
While the hallmark symptom is the increase in heart rate, POTS is a collection of symptoms. These include:
- Sudden change in blood pressure
- Nausea
- Dizziness / Vertigo
- Anxiety / Palpitation
- Sweating
- Tremulousness
- Hyperventilation / Dyspnoea
- Weakness
- Sleep disorder
- Fatigue
- Headache
- Exercise intolerance
POTS and Exercise
While there is no cure for POTS exercise is recommended to help improve physical capacity while minimising symptom exacerbation.
Exercising with POTS can be challenging due to a high exercise intolerance and debilitating post-exercise fatigue. As patients find it difficult to exercise, they can become increasingly deconditioned.
One study using a Dallas Protocol, which is a protocol that was developed for the management of POTS found that following a structured exercise program involving a combination of aerobic exercise and resistance training can improve orthostatic and exercise tachycardia, symptoms and quality of life. This improvement is related to an increase in the size and strength of contraction of the heart and improved ability of the body to circulate the blood back up to the heart more efficiently.

Exercise conditioning is a fundamental aspect of postural orthostatic tachycardia syndrome treatment and it is a recommendation for all patients to start on a gradual physical exercise regimen. Given that most exercise is completed upright and therefore a trigger for symptoms, beginning with a supervised low-intensity program focused on avoiding upright positioning with incremental progression over 3 months has been demonstrated to improve symptoms. It is best to start with exercise that is either horizontal (such as swimming), reclined (such as a recumbent bike), or seated with legs elevated (such as rowing). As there is often an impaired venous return in POTS (the return of blood back to the heart) exercises avoiding upright positioning can promote better venous return by reducing the distance bloods needs to travel against gravity, thus improving circulation efficiency and improving symptoms.
Exercise Physiology and POTS
Due to many clients with POTS struggling with standing and exercise intolerance, the goal of therapy would be to improve these intolerances. Exercise is never a one-size fits all situation, and POTS management is no different. Completing an individualised program that addresses your symptom specific needs, co-morbities and is flexible based on how you present to an exercise session is essential. Having a planned program run by one of our exercise physiologists will ensure that postural changes are minimised during your sessions to enable safe exercise that will also help to manage your symptoms. Again, while there is not cure for POTS exercise when done in a way that is tolerated is a great way to improve symptoms and help you get back to doing those things you love.
References:
A K Agarwal, R Garg, A Ritch, P Sarkar, Postural orthostatic tachycardia syndrome, Postgraduate Medical Journal, Volume 83, Issue 981, July 2007, Pages 478–480, https://doi.org/10.1136/pgmj.2006.055046
Fu, Q., VanGundy, T.B., Shibata, S., Auchus, R.J., Williams, G.H. and Levine, B.D., 2011. Exercise training versus propranolol in the treatment of the postural orthostatic tachycardia syndrome. Hypertension, 58(2), pp.167-175.
Garland, E.M., Celedonio, J.E. & Raj, S.R. Postural Tachycardia Syndrome: Beyond Orthostatic Intolerance. Curr Neurol Neurosci Rep 15, 60 (2015). https://doi.org/10.1007/s11910-015-0583-8
Zhao S, Tran VH. Postural Orthostatic Tachycardia Syndrome. [Updated 2023 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541074/