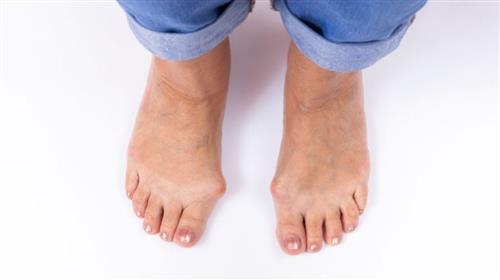
The Issue with Diabetes
The Issue with Diabetes
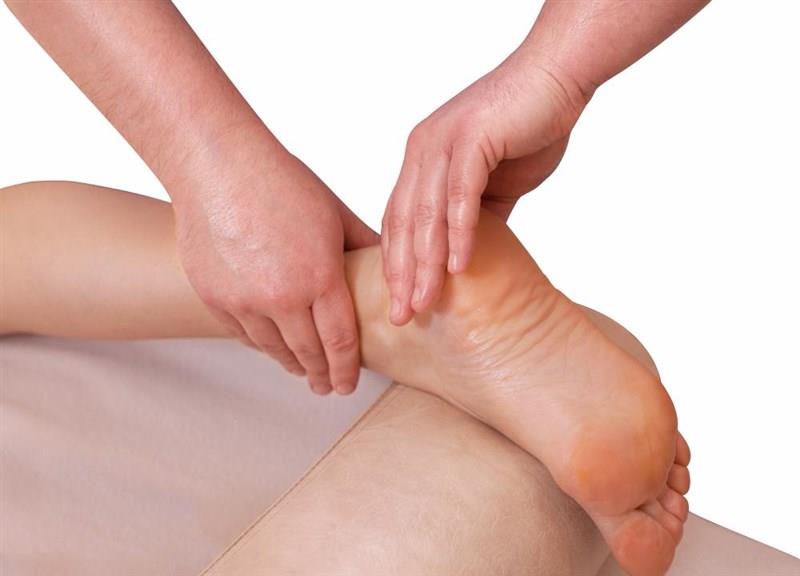
Diabetes can cause many problems in the feet, including ulcers and nerve damage that can lead to amputation. Diabetic foot ulcers are among the most common and severe infections associated with diabetes, resulting from ulcers that may develop into life-threatening limb loss. Painful nerve damage is a common problem affecting up to half of all people with diabetes and can result in pain, tingling, and numbness in the feet. Podiatrists play an essential role in preventing complications such as amputation by providing education and clinical care for those at risk for developing Charcot’s foot: patients who have had a total lower limb amputation due to diabetic vascular disease.
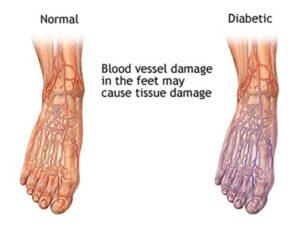
High glucose levels can cause permanent damage to blood vessels and nerves, resulting in diabetic neuropathy, which, in unmanaged severe cases, may lead to a condition called Charcot’s foot.
Diabetic foot is a serious complication of diabetes that, in severe cases, can lead to amputation. It’s caused by nerve damage and poor circulation, which in turn leads to ulcers on the feet. High glucose levels can cause permanent damage to blood vessels and nerves, resulting in diabetic neuropathy, which may lead to a condition called Charcot’s foot.
Charcot foot is a condition where ulcers develop on the bottom of your feet due to peripheral neuropathy (nerve damage). Peripheral neuropathy is a common complication of diabetes that causes numbness or pain in your hands and feet. It affects about 50 per cent of people with Type 2 diabetes on average, about ten years from diagnosis; however, it can be much sooner if the condition does not have good management.
Diabetic foot infections are one of the most common and severe conditions associated with diabetes, resulting from ulcers that may develop into life-threatening diseases and limb loss.
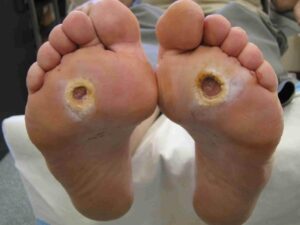 Diabetic foot infections are one of the most common and severe conditions associated with diabetes, resulting from ulcers that may develop into life-threatening limb loss.
Diabetic foot infections are one of the most common and severe conditions associated with diabetes, resulting from ulcers that may develop into life-threatening limb loss.
Diabetic foot infections can be caused by poor circulation, neuropathy, and peripheral vascular disease (PVD).
Painful nerve damage is a common problem affecting up to half of all people with diabetes and can result in pain, tingling, and numbness in the feet.
Painful nerve damage is a common problem affecting up to half of all people with diabetes and can result in persistent pain, tingling, and numbness in the feet. Diabetic neuropathy is a nerve disorder that can cause numbness, tingling, or burning sensations in the extremities (hands and feet). The most common symptom is painless loss of success on the soles of your feet, which may lead to ulceration and amputation if not cared for.
The exact cause of this type of nerve damage isn’t known, but it’s thought that high blood glucose levels may affect how nerves work by damaging their myelin sheaths (coverings). This makes them more likely to be damaged by other factors, such as poor blood flow through arteries carrying oxygenated blood into tissue cells via tiny capillaries under the skin surface called perforators. These supply oxygenated blood directly into nerves at various points along the length. Hence, they can function correctly without having adequate supplies available locally within each cell (which would otherwise occur if healthy).
Foot ulceration is a common complication of diabetes mellitus and is associated with a high risk of lower extremity amputation.
Foot ulceration is a common complication of diabetes mellitus and is associated with a high risk of lower extremity amputation. Foot ulceration occurs in 20–40% of people with diabetes mellitus. The pathophysiology of foot ulcers has been linked to peripheral neuropathy, peripheral vascular disease, and kidney disease.
Depending on the severity of your diabetes, daily foot inspections should be done as part of every person’s daily routine. Self-examinations are performed for abnormalities such as sores, blisters, redness, calluses, or ingrown toenails.
In addition to podiatry examinations, daily foot inspections should be part of every person’s daily routine. Self-examinations are performed for abnormalities such as sores, blisters, redness, calluses, or ingrown toenails. This self-examination is simple and easy to follow:
- Check your feet in good light with a mirror, or ask someone else to help you check all areas of your feet (including between toes) for signs of infection or injury.
- Look at the soles of each foot carefully; look at both sides of each toe individually. Inspect between toes using a magnifying glass if needed; look at the heel area, too! Inspect the skin around the nails; make sure there aren’t any cuts or splits in the skin here, which could lead to developing an infection.
Podiatrists work with primary care physicians and wound care specialists to deliver the best care for diabetic patients.
Podiatrists are experts in foot health and can help patients with diabetes avoid complications. As part of a team that includes primary care physicians and wound care specialists, podiatrists are essential in treating diabetic foot problems. Podiatrists are trained to diagnose and treat foot conditions, including infections; advise and, in some cases, prescribe medications for pain; provide surgical procedures; insert orthotics into shoes to correct biomechanical abnormalities; test and manage nerve damage associated with peripheral vascular disease; remove calluses from the bottom of your feet using professional medical equipment or scraping devices; remove corns; and treat hammertoes and complications arising from bunions.
Podiatrists are essential in treating and preventing diabetic foot complications, including avoiding amputation or managing people who have undergone these procedures, Charcot foot management, peripheral neuropathy, ulceration, and infection prevention through professional foot care.
 Podiatrists are trained to treat and prevent diabetic foot complications. They can help you manage your diabetes and the associated risks of wounds, ulcerations, and amputations.
Podiatrists are trained to treat and prevent diabetic foot complications. They can help you manage your diabetes and the associated risks of wounds, ulcerations, and amputations.
If you have diabetes, it’s essential to see a podiatrist in Adelaide regularly for checkups that include:
- Foot examination
- Blood flow testing
- Sensation testing
- Care, including skin and nail management
- Footwear education
- Advice regarding effective self-management techniques
Proper footwear is an essential tool for preventing complications for people with diabetes. Shoes should fit comfortably right out of the box.
Proper footwear is an essential tool for preventing complications for people with diabetes. Shoes should fit comfortably right out of the box.
- Shoes that have soft soles and plenty of room for your toes are good choices for people who have diabetic foot problems.
- This assists in reducing the risk of developing foot skin issues and the complications that arise from them.
- Make sure your shoes have plenty of room at the end of your longest toe and are comfortable when you walk in them or stand up straight on both feet.
Podiatry care and management are critical in the direction of diabetic foot care.
As you can see, podiatrists are essential in treating and preventing diabetic foot complications. If you have questions about any of these conditions or want to make an appointment with Inertia Podiatrists, don’t hesitate to call our clinic today at (08 8359 2022) or book online!